Forget hand hygiene and hotel duvet germs; today, we’re diving into the fascinating world of gut bacteria. With the increasing buzz around probiotics and their impact on overall health, researchers are now examining how manipulating the gut microbiome could affect individuals with inflammatory bowel disease (IBD), such as Crohn’s disease. But are probiotics and probiotics truly a game-changer for Crohn’s? The answer is… maybe. While there’s no definitive answer, let’s explore the potential benefits, drawbacks, and all-around intrigue of probiotics for Crohn’s.
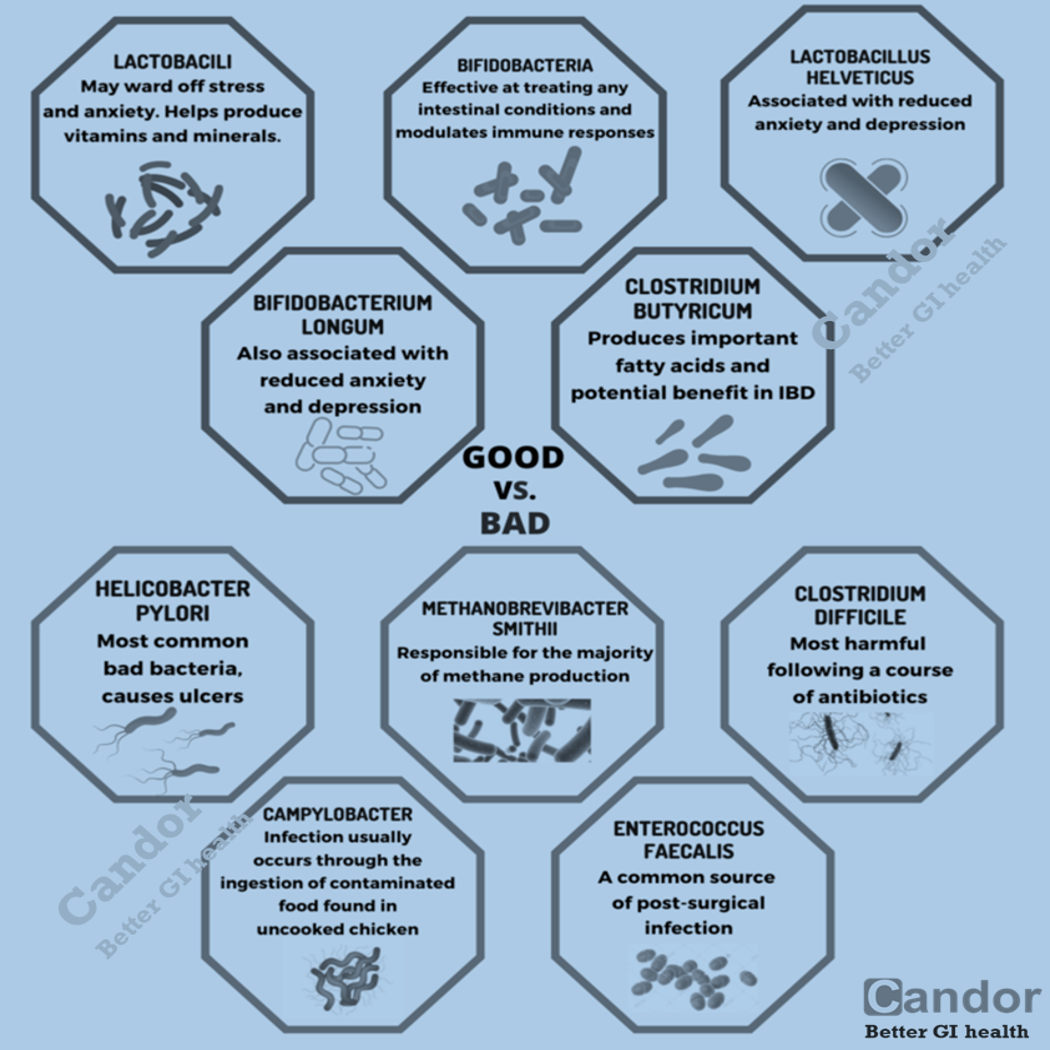
First, let’s understand what probiotics actually do. Inside your intestines, a bustling community of both good and bad bacteria coexist. When the good bacteria dwindle, the bad bacteria can take over, leading to unpleasant symptoms like gas, bloating, diarrhea, and other bathroom-related struggles. Probiotics, the superheroes of the bacterial world, are believed to replenish the friendly bacteria in your gut, fostering a healthier balance and providing various health benefits. By consuming probiotics through food or supplements, you can contribute to a more favorable gut microbiome, where the good bacteria overpower the bad, preventing their proliferation and potentially easing Crohn’s symptoms.
But is it worth your time and effort? Let’s dive into the effects of probiotics on your health.
Pinpointing the benefits of probiotics can be tricky because the existing research is inconclusive. Most studies conducted on probiotics for IBD, including Crohn’s, have been small-scale, so it’s not time to either embrace or dismiss probiotics altogether. Although probiotics have shown positive results in relieving bloating, pain, and diarrhea for individuals without conditions like Crohn’s, their impact on GI symptoms of Crohn’s disease isn’t always straightforward. While one review indicated that probiotics were effective for ulcerative colitis, another form of IBD, they had no significant effect on Crohn’s. However, this doesn’t mean probiotics are a lost cause. It could be due to poor absorption or the wrong strains being used.
But hold on, it’s not all doom and gloom. Some evidence suggests that probiotics might be beneficial for individuals in the early stages of Crohn’s disease. However, further research is necessary to validate these claims. The scientific community is intrigued by the potential of probiotics for IBD, thanks to their easy administration, relatively low cost, and the prospect of relieving symptoms. As more research unfolds, we may gain more concrete evidence supporting the benefits of probiotics. In the meantime, consult your doctor before hopping on the probiotics bandwagon.
When it comes to choosing probiotics, one study with promising results involved a probiotic containing Bifidobacterium longum and the prebiotic Synergy 1. While it’s not the only option, discussing the possibility of a synbiotic mix with your doctor could be worthwhile.
While probiotic supplements are available, numerous fermented foods also provide probiotics. However, be cautious with store-bought fermented products, as processing can diminish the levels of beneficial bacteria. Look for labels that indicate “live cultures” or consider making your own homemade yogurt for a reliable probiotic source.
Now, let’s address some safety tips with probiotics. Unfortunately, there’s evidence suggesting that probiotics could worsen Crohn’s symptoms. Since the digestive tract is already inflamed, introducing any type of bacteria could potentially trigger a flare-up. A small study discovered that individuals with Crohn’s fared better with a placebo than with probiotics. Some anecdotal evidence also suggests that probiotics could lead to infection in individuals with severe Crohn’s or those on immunosuppressive medications. Overall, the chances of probiotics causing harm or providing significant benefits are low. To ensure your well-being, consult your doctor before incorporating probiotics into your routine.
Now, let’s shift gears and talk about prebiotics.
Prebiotics show more promise in the realm of Crohn’s disease. These indigestible carbohydrates naturally found in various fruits, vegetables, and plant foods serve as fuel for the good bacteria in your gut, promoting their growth and overall health. A small three-week study involving individuals with Crohn’s revealed that consuming 15 grams per day of oligofructose and inulin (prebiotic natural fibers) led to a significant reduction in disease activity. Although small-scale, this study offers hope for the potential benefits of prebiotics. Finding natural prebiotics is relatively easier in grocery stores. Chicory root, Jerusalem artichokes, garlic, onions, oats, apples, asparagus, and bananas are all excellent sources of the prebiotic fiber inulin. Incorporate these into your regular diet and observe if they have any beneficial effects.
What about safety tips with prebiotics? Since prebiotic fibers remain undigested until they reach the colon, they can contribute to gas, bloating, and discomfort. Moreover, if you’re following a low-FODMAP diet for Crohn’s, finding suitable natural prebiotic sources might be challenging. If you’re well aware of your food triggers and can tolerate garlic, onions, and similar foods, trying prebiotics should generally be safe. Nevertheless, consult your doctor for personalized guidance.
Let’s not forget about synbiotics, a combination of prebiotics and probiotics. With synbiotics, you get the best of both worlds: the good bacteria and the fuel to nourish them, all in one package. While one preliminary study touted synbiotics as an effective Crohn’s treatment, another found no significant difference. Interestingly, a study involving children with Crohn’s indicated that synbiotics were not effective in their case. So, what’s the bottom line? Keep in mind that these studies are limited in scope, and more research is required. However, for adults with Crohn’s, synbiotics have shown some promise.
What about the intriguing world of postbiotics?
The true wonders of gut bacteria don’t solely lie in the microorganisms themselves, but rather in the by-products they produce through their metabolic processes. It may not sound appealing, but these waste products can actually be beneficial to us. Let’s take bifidobacteria as an example. When they consume fiber, they generate short-chain fatty acids as waste. Surprisingly, these fatty acids play a crucial role in enhancing our immune function and fortifying the intestinal barrier. Recognizing the potential of these end-products, researchers have started exploring the idea of delivering them directly to the gut. This innovative approach offers a way to bypass the challenges of introducing live organisms into the gut unscathed and instead directly provide the benefits of these metabolic by-products. Moreover, this method could be particularly valuable for individuals with compromised immune systems, allowing them to reap the advantages of probiotics without the associated risks.
In summary, postbiotics represent an exciting avenue to harness the benefits of gut bacteria. By focusing on the waste products they produce, we can potentially unlock new possibilities for improving our overall health and well-being.
Now, let’s delve into the curious realm of fecal transplants.
Yes, you read that right. Scientists are experimenting with the transfer of fecal matter from one person to another as a potential treatment. This peculiar approach aims to bypass gastric acids and directly introduce healthy bacteria to an unhealthy bowel. Before you start seeking out generous poop donors, it’s important to note that fecal transplants are not yet FDA-approved for treating IBD. Nevertheless, ongoing research may eventually make this an option worth considering.
In conclusion, although it would be wonderful to proclaim that both prebiotics and probiotics work wonders for relieving Crohn’s, the reality is more complex. Currently, there is no definitive evidence to support the efficacy of probiotics for Crohn’s, and the likelihood of them worsening symptoms is relatively low. On the other hand, prebiotics and synbiotics show slightly more promise.
Remember, always consult your doctor before incorporating any dietary changes. Keep in mind that the FDA doesn’t rigorously test dietary supplements for safety and efficacy like it does with food and drugs. It’s essential to conduct thorough research and choose reputable brands that undergo third-party testing. So, embrace your gut bacteria adventure cautiously, and let science guide you on your journey to optimal gut health.
References:
- Fujimori S, et al. (2007). “High dose probiotic and prebiotic cotherapy for remission induction of active Crohn’s disease.” Journal of Gastroenterology and Hepatology.
- Hansen R, et al. (2011). “Synbiotics for inflammatory bowel disease: useful in adults but problematic in pediatrics.” British Society of Paediatric Gastroenterology, Hepatology and Nutrition.
- Lichtenstein L, et al. (2016). “Probiotics and prebiotics in Crohn’s disease therapies.” Best Practice and Research: Clinical Gastroenterology.
- Prantera C, et al. (2002). “Ineffectiveness of probiotics in preventing recurrence after curative resection for Crohn’s disease: a randomised controlled trial with Lactobacillus GG.” BMJ: Gut.