This comprehensive exploration aims to deepen our understanding of how to manage IBS pain and cramps, shedding light on the underlying causes and distinctive characteristics. Furthermore, it serves as a guide on when seeking the expertise of a healthcare provider becomes essential for effective care.
Abdominal pain, a hallmark symptom of Irritable Bowel Syndrome (IBS), often proves elusive and challenging to predict. The subjective nature of IBS pain – its diverse sensations, triggers, and specific locations – presents a unique landscape for each individual. Recent studies delve into the intricate relationship between the severity of IBS symptoms and female sex hormones, adding another layer of complexity to this prevalent condition.
Unraveling the Complex Causes of IBS Pain
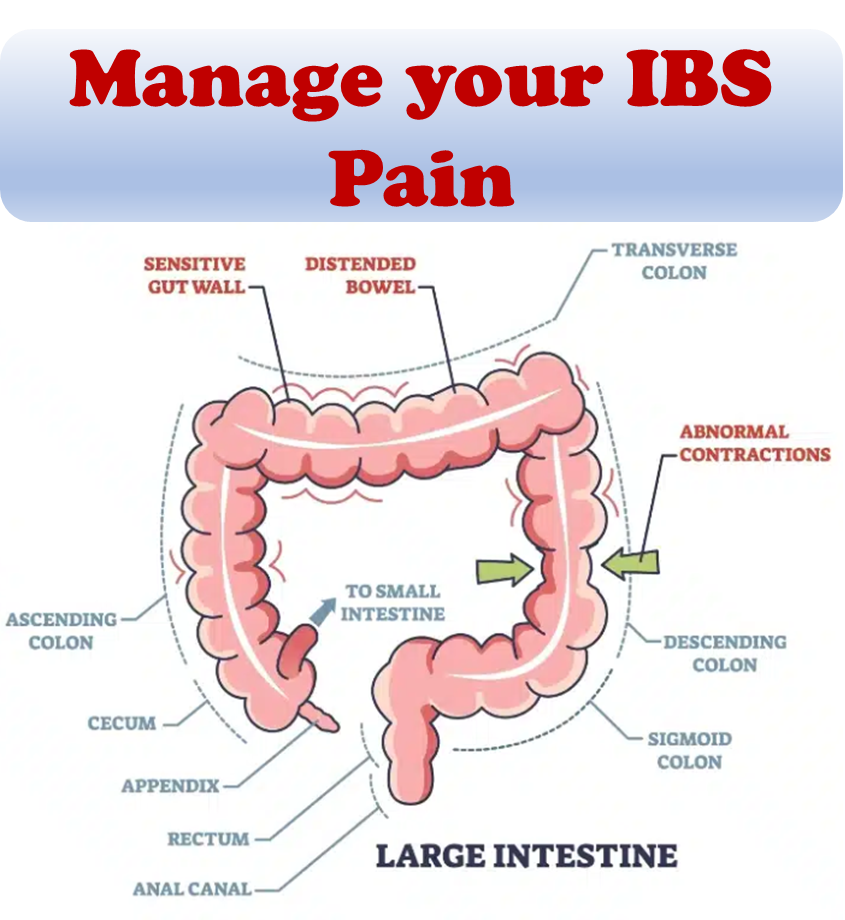
To comprehend IBS pain fully, it is vital to recognize its chronic nature and the visceral origin within the internal organs, particularly the intestines. This visceral pain is functional, emphasizing that despite normal imaging results, the pain is genuine. Individuals with IBS exhibit heightened sensitivity, where ordinary levels of gas or intestinal movement trigger pain-sensing nerve receptors more intensely than usual. This phenomenon, known as central sensitization, leads the brain to amplify pain messages, causing routine sensations like digestion to be perceived as painful. IBS is aptly labeled as a central sensitivity syndrome.
Addressing this complexity, treatment plans may incorporate certain antidepressants, such as Elavil (amitriptyline) or Pamelor (nortriptyline). Beyond regulating gut nerve receptors, these medications also play a crucial role in reducing anxiety, a common companion to IBS that can further exacerbate gut sensitivity. It’s imperative for individuals to maintain open communication with their healthcare providers to ensure accurate diagnoses and effective treatment plans.
Understanding the Multifaceted Nature of IBS Pain
Describing the sensation of IBS pain often revolves around the term “cramps,” encompassing a spectrum from sharp stabbing to constant aching or painful spasms. Tenderness upon touch and bloating add layers to this complex experience. The severity of IBS pain spans from mild, nagging discomfort to severe, potentially crippling pain. Importantly, its intensity may fluctuate throughout the day, presenting challenges in planning daily activities.
People with IBS typically experience pain at least once a week, with the frequency varying significantly between individuals. For some, the pain becomes an unwavering companion, while others may have intermittent episodes or pain-free days. The location of the pain spans a considerable area, from the chest to the pelvis, covering different segments of the digestive organs.
By comprehending the nuanced facets of IBS pain and adopting a holistic approach to management, individuals can navigate the challenges posed by this condition more effectively, enhancing their overall quality of life.
Triggers of IBS Pain: Unmasking the Culprits
Identifying triggers for IBS pain is essential in managing the condition. Stress, irregular eating habits, specific foods (such as spicy or fatty options), and intense exercise are known culprits. The evolving diagnostic criteria highlight the connection between IBS pain and defecation, emphasizing a nuanced relationship rather than a simplistic improvement or worsening with bowel movements.
Comprehensive Insights into Other IBS Symptoms
Beyond pain, IBS manifests in a spectrum of symptoms, including constipation, diarrhea, mixed bowel habits, passing mucus during bowel movements, a sensation of incomplete evacuation, and abdominal bloating. Recognizing and understanding these symptoms contribute to a comprehensive grasp of IBS, allowing for more targeted interventions.
How Women Navigate the Landscape of IBS Pain
While IBS symptoms vary among individuals, gender differences come to the forefront, with women experiencing IBS in distinct ways compared to men. Not only is IBS more prevalent in females, but they also report more severe abdominal pain and symptoms related to constipation. The fluctuation of IBS symptoms during different menstrual phases, particularly worsening during periods, is a common experience for women.
Interestingly, those who are pregnant or have completed menopause may observe improvements in their IBS symptoms. Research suggests that female sex hormones, specifically progesterone and estrogen, play a pivotal role in influencing bowel function, pain perception, and gut flora.
Holistic Strategies for Relieving IBS Pain
For individuals grappling with IBS, a holistic approach to symptom management is essential. Regular monitoring of symptoms, daily bowel habits, and factors influencing the condition provides valuable insights. Treatment strategies for IBS pain encompass dietary changes, medication options, and psychosocial therapy.
Dietary Changes: Strategic modifications, such as avoiding gas-inducing foods and increasing fiber intake, can contribute to alleviating IBS pain.
Medication Options: Depending on individual symptoms, various medications, including anticholinergic drugs, low-dose antidepressants, lubiprostone, linaclotide, alosetron, and eluxadoline, may offer relief.
Psychosocial Therapy: Cognitive Behavioral Therapy (CBT) or hypnotherapy stands as effective avenues for individuals to cope with the challenges posed by IBS symptoms.
References:
- “Definition and Facts for Irritable Bowel Syndrome”. NIDDKD. February 23, 2015.
- Chey WD, Kurlander J, Eswaran S (March 2015). “Irritable bowel syndrome: a clinical review”. JAMA.
- Lacy BE, Pimentel M, Brenner DM, et al. (2021) “ACG clinical guideline: management of irritable bowel syndrome.” American Journal of Gastroenterology.
- Hou JK, Lee D, Lewis J (October 2014). “Diet and inflammatory bowel disease: review of patient-targeted recommendations”. Clinical Gastroenterology and Hepatology (Review).