FODMAPs that are present in gluten-containing grains have been identified as a possible cause of gastrointestinal symptoms in people with non-celiac gluten sensitivity, in place of, or in addition to, gluten and other proteins in gluten-containing cereals, named amylasetrypsin inhibitors (ATIs). The amount of fructans in these cereals is small. In rye they account for 3.6%–6.6% of dry matter, 0.7%–2.9% in wheat, and barley contains only trace amounts. They are only minor sources of FODMAPs when eaten in the usual standard amounts in the daily diet. Wheat and rye may comprise a major source of fructans when consumed in large amounts.
In a 2018 double-blind, crossover research study on 59 persons on a gluten-free diet with challenges of gluten, fructans or placebo, intestinal symptoms (specifically bloating) were borderline significantly higher after challenge with fructans, in comparison with gluten proteins. Although the differences between the three interventions was very small, the authors concluded that fructans are more likely to be the cause of gastrointestinal symptoms of non-celiac gluten sensitivity, rather than gluten. In addition, fructans used in the study were extracted from chicory root, so it is unclear whether the wheat fructans produce the same effect.
A 2018 review concluded that although fructan intolerance may play a role in non-celiac gluten sensitivity, it only explains some gastrointestinal symptoms, but not the extra-digestive symptoms that people with non-celiac gluten sensitivity may develop, such as neurological disorders, fibromyalgia, psychological disturbances, and dermatitis; and that FODMAPs cause digestive symptoms when the person is hypersensitive to luminal distension.
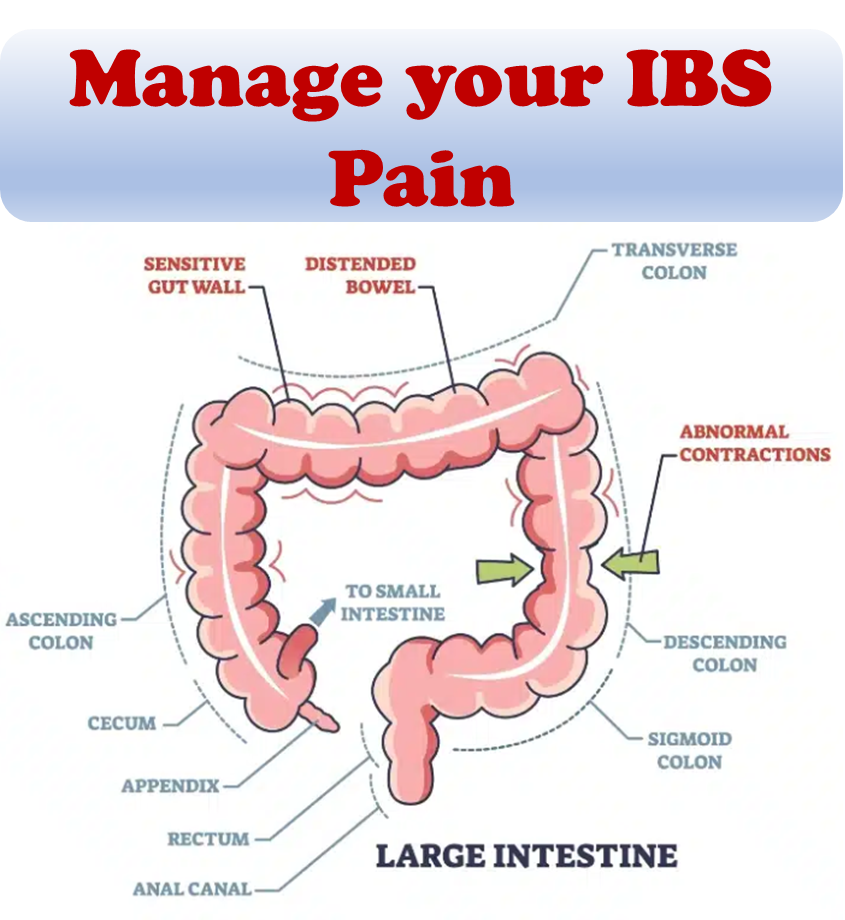
A 2019 review concluded that wheat fructans can cause certain IBS-like symptoms, such as bloating, but they are not likely to cause immune activation nor extra-digestive symptoms since, in fact, many people with non-celiac gluten sensitivity report resolution of their symptoms after removing gluten-containing cereals while they continue to eat fruits and vegetables with high FODMAPs content in their diet.
Source: National Institutes of Health