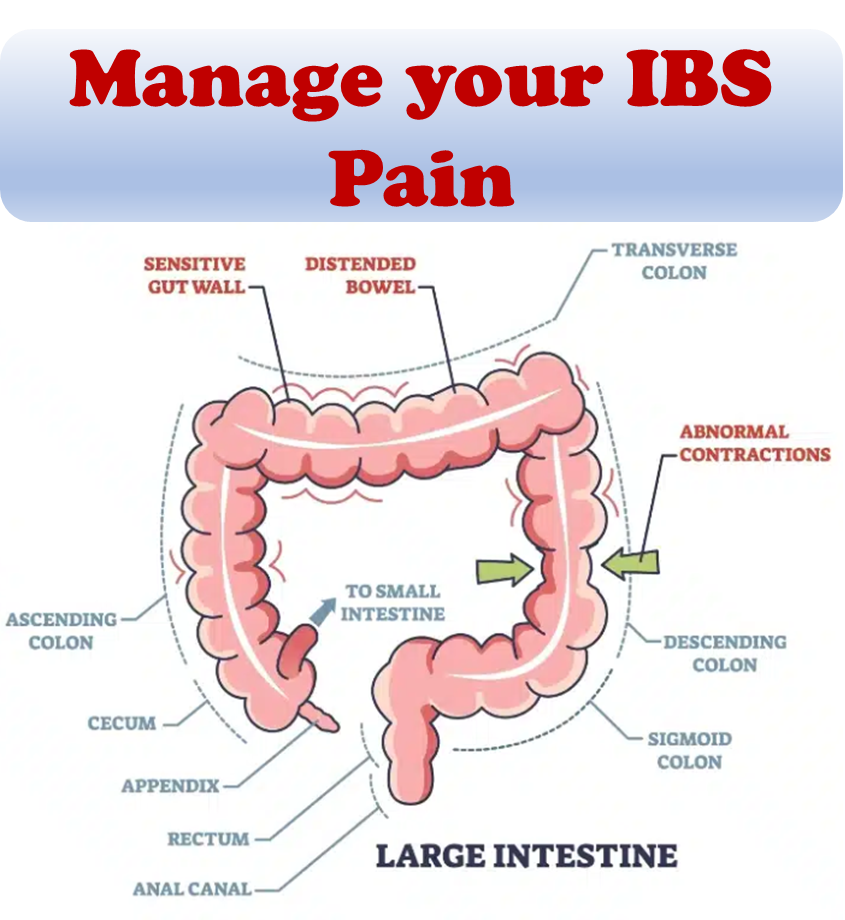
If you’re seeking ways to alleviate and control the distressing symptoms of Irritable Bowel Syndrome (IBS), understanding the impact of specific foods is crucial. Nutrition and lifestyle strategies can play a vital role in managing IBS symptoms, improving your overall well-being, and optimizing digestive health. Discovering the right foods for IBS can be a game-changer, as triggers can vary from person to person. This article outlines effective strategies and dietary choices to help you navigate the world of IBS foods and find relief.

Here are some strategies and thoughts on IBS foods to incorporate into your IBS management plan
- Stick to regular mealtimes and practice thorough chewing while eating. Opt for smaller, more manageable portions to aid digestion and minimize discomfort.
- Stay adequately hydrated by consuming a minimum of 8 cups (2 liters) of fluids per day. Opt for water, herbal teas, and broths to maintain hydration levels.
- Consider a short-term low FODMAP diet to identify specific food triggers. FODMAPs are carbohydrates that can potentially exacerbate gut symptoms. High FODMAP foods include apples, onions, garlic, wheat, lactose, and sugar alcohols.
- Space out your fruit intake by at least 2-3 hours and limit yourself to one fruit portion per meal or snack.
- Opt for cooked vegetables over raw ones, as they are easier to digest.
- Choose easily digestible protein sources such as eggs, chicken, turkey, fish, extra-firm tofu, and plain lactose-free Greek yogurt. Opt for cooking methods like baking, roasting, steaming, boiling, or sautéing, using lower-fat options to minimize discomfort.
- If you experience constipation, introduce certain fiber sources into your diet, such as flaxseeds, oats, inulin, or psyllium. However, avoid highly fermentable fibers like wheat bran and prunes, as they can trigger gas and abdominal pain.
- Limit the consumption of gas-producing vegetables and legumes, including broccoli, cauliflower, cabbage, Brussels sprouts, chickpeas, lentils, and black beans, if they worsen your symptoms.
- Restrict your intake of coffee and strong caffeinated teas (black and green) to a maximum of 3 cups per day.
- Minimize your consumption of alcohol, carbonated drinks, spicy foods, and deep-fried, greasy options like French fries, pizza, hamburgers, and tempura.
- Avoid sugar alcohols and artificial sweeteners such as sorbitol, mannitol, xylitol, maltitol, and erythritol, especially if you experience diarrhea. Be cautious of natural sources of these compounds, including prunes, cauliflower, mushrooms (except oyster mushrooms), and sugar-free candies and gums.
- Consider a short-term trial of a daily probiotic for at least one month, monitoring its impact on your symptoms. Visit probioticchart.ca for a comprehensive list of evidence-based probiotics in Canada. Consult your doctor, pharmacist, or registered dietitian to ensure it’s suitable for your condition.
- Rule out gluten intolerance and celiac disease, as some individuals may have a sensitivity to wheat carbohydrates (FODMAPs) rather than the protein (gluten). For instance, many people with suspected gluten intolerance tolerate 100% sourdough wheat bread (low FODMAP) but not regular wheat bread.
- Incorporate regular physical activity into your routine to reduce gas, bloating, stress, and anxiety—common triggers for gut symptoms. Seek guidance from your doctor, kinesiologist, or physiotherapist to determine the appropriate level of exercise for your needs.
- Prioritize stress and anxiety management, as the brain-gut connection is well-established. Implement stress-reducing techniques such as spending time in nature, listening to calming music, taking power naps, cooking, practicing meditation, tai chi, yoga, engaging in writing or reading, enjoying massages, and exploring therapy options. Psychological therapies like biofeedback, cognitive-behavioral therapy (CBT), and gut-directed hypnotherapy may also be beneficial.
By implementing these nutrition and lifestyle strategies tailored to IBS, you can regain control over your symptoms and improve your overall quality of life. Remember, finding the right combination of IBS foods and practices is a personal journey, and collaborating with healthcare professionals will greatly enhance your success in managing IBS effectively.
References:
- Williams CE, Williams EA, Corfe BM (October 2018). “Vitamin D status in irritable bowel syndrome and the impact of supplementation on symptoms: what do we know and what do we need to know?” (PDF). European Journal of Clinical Nutrition.
- Moayyedi P, Quigley EM, Lacy BE, Lembo AJ, Saito YA, Schiller LR, Soffer EE, Spiegel BM, Ford AC (September 2014). “The effect of fiber supplementation on irritable bowel syndrome: a systematic review and meta-analysis”. The American Journal of Gastroenterology.
- Andoh A, Tsujikawa T, Fujiyama Y (2003). “Role of dietary fiber and short-chain fatty acids in the colon”. Current Pharmaceutical Design (Review).
- Barbara G, et al. (2009). “Aminosalicylates and other anti-inflammatory compounds for irritable bowel syndrome”. Digestive Diseases.