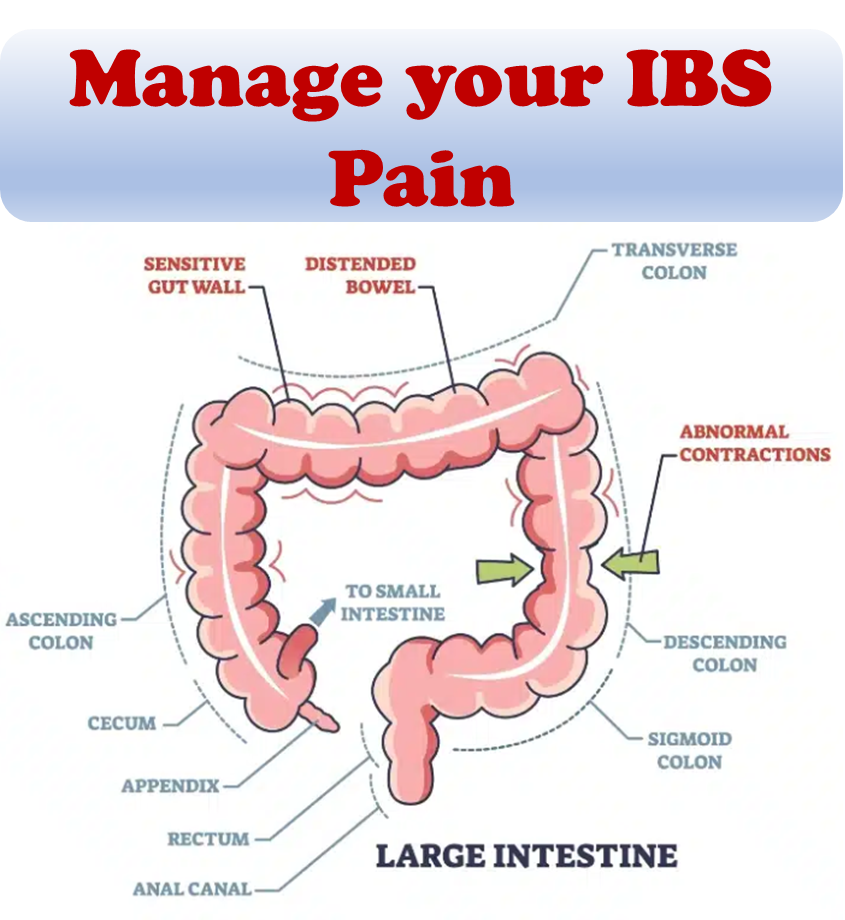
Diet appears to play an important role in IBS, with up to 84 percent of sufferers reporting food‐related symptoms, especially for foods containing fermentable carbohydrates and fats. Most patients are keen to explore dietary options, with almost 63% wanting to know what foods to avoid and about 70% having already tried to modify their diet.
Traditional dietary advice and its principles include healthy eating and lifestyle management, eating regular meals and adjusting levels of fiber, fluid, alcohol, caffeine, fat and spices that may exacerbate symptoms. These recommendations are based primarily on known physiological effects of different foods in the GI tract, as well as on clinical experience, rather than on results from randomized controlled studies.
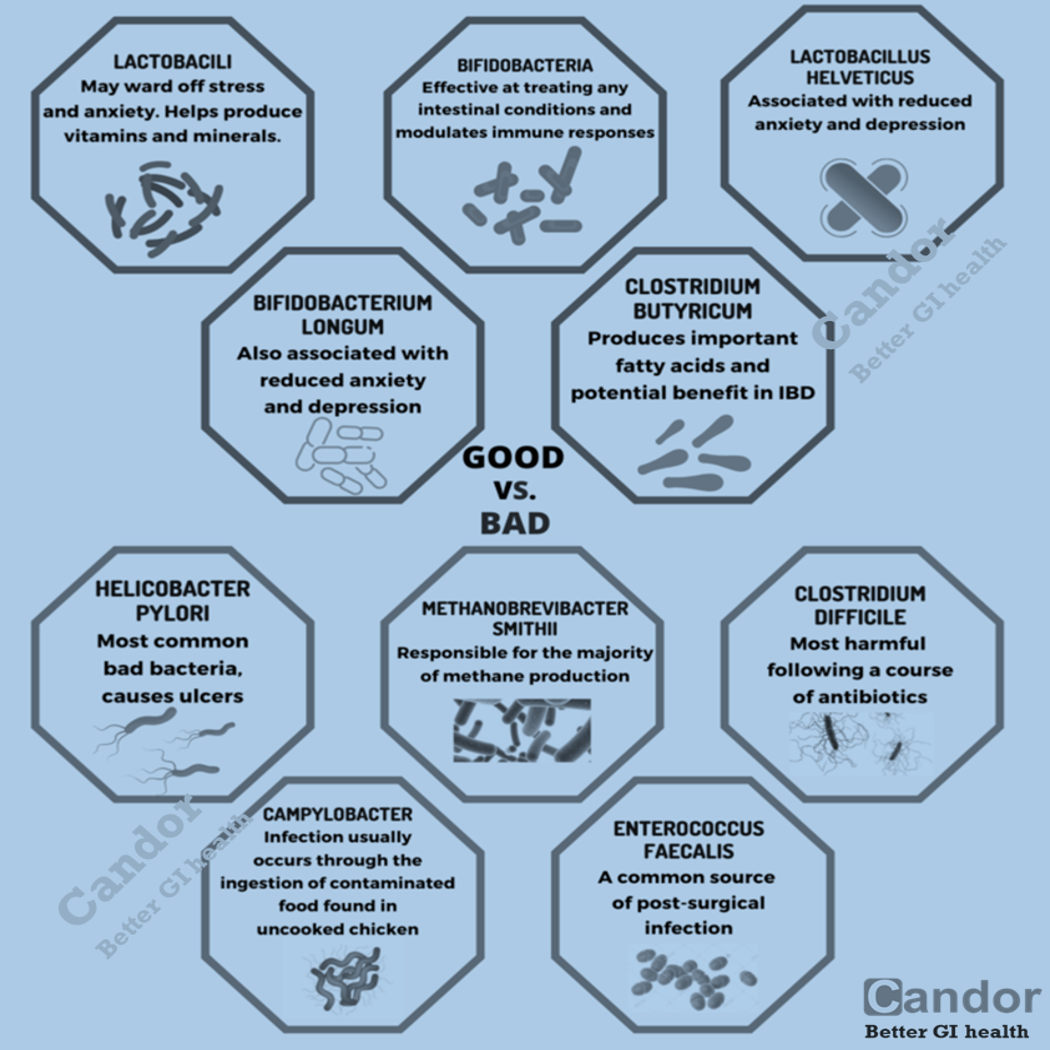
There is insufficient evidence of the effect of fibers other than psyllium, and recent studies on prebiotics suggest a limited effect. Probiotic trials continue to provide varying results, with some probiotic strains exhibiting beneficial effects, whereas others show no effect. Recent trials have also confirmed the clinical effectiveness of a low FODMAP diet for IBS. Although gluten sensitivity has also been recently investigated, its presence cannot be confirmed yet because of the presence of other potential contributing compounds in wheat. Studies also suggest a potential beneficial effect of peppermint oil, which warrants further research.
For a sample of controlled Bloating, pain, and flatulence were the symptoms showing greatest improvement on the low-FODMAP diet. Patients of all IBS subtypes had better stool consistency while on the low-FODMAP diet.
SUMMARY:
It is clear that a low FODMAP diet has a beneficial effect in a majority of patients with IBS. Probiotics also have great potential in the management of IBS; however, it is still unclear which strains and doses are the most beneficial. Further research is needed on the effect of different fibers, or combinations of fibers, in IBS.
Follow us on:
http://www.facebook.com/getcandorapp