Cognitive behavioral therapy (CBT) is a type of psychotherapy originally developed and used to treat mental health issues such as depression and anxiety. CBT as a treatment tends to be short-term and collaborative. The patient and therapist work together to address symptoms, which typically includes both in-session and at-home practice. CBT targets problem areas through the use of specific cognitive and behavioral techniques.
- CBT is grounded in the belief that our thoughts (cognitions), feelings, and behaviors are all related. More specifically, unhelpful thoughts negatively impact how we feel and these negative feelings can impact how we behave.
- By engaging in unhelpful behaviors, we reinforce negative thoughts. CBT aims to help by evaluating and modifying our thoughts and behaviors to make them more helpful, and to improve our emotional state.
- Negative emotions (e.g., fear, frustration) put our bodies into a state of autonomic arousal, which is sometimes called the “Fight or Flight Response.” Increases in stress hormones, blood pressure, heart rate, and changes in digestive function are all part of this crucial evolutionary mechanism meant to keep us safe from threats to our survival.
- However, the fight or flight response can be triggered even in response to stressful events that are not an actual threat to physical safety, such as nervousness when preparing to give a speech or in response to abdominal discomfort.
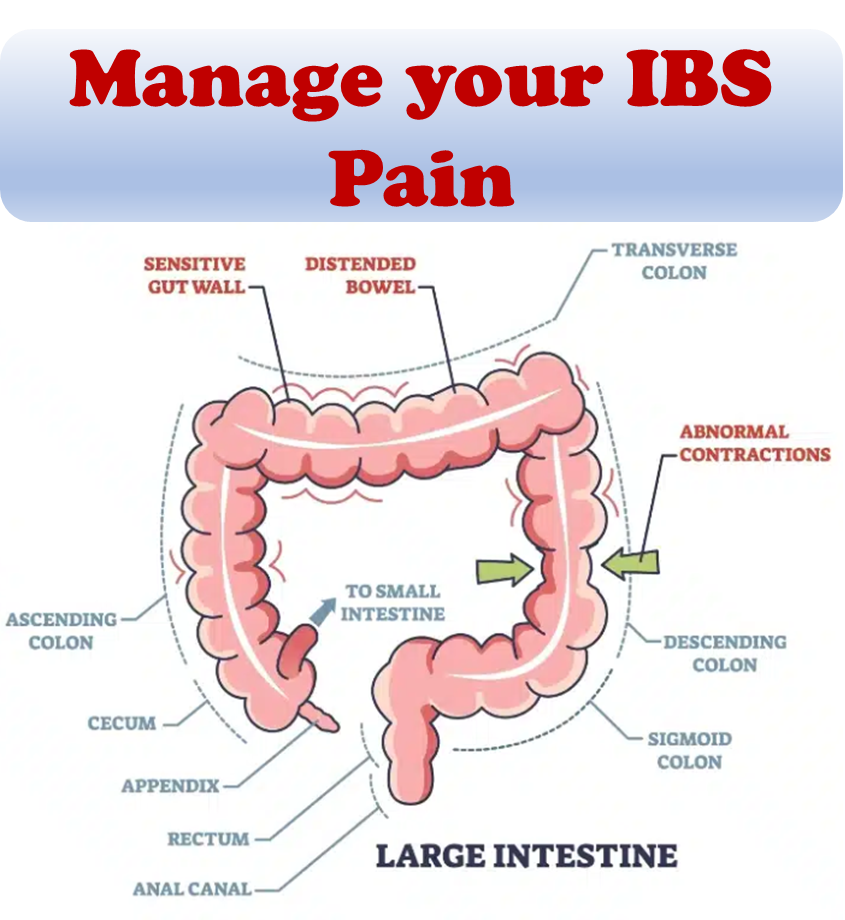
- IBS can induce chronic stress and uncomfortable physical symptoms – this puts the body regularly in a state of autonomic arousal, potentially worsening the physical symptoms.
- The body also has a physiological response called the parasympathetic nervous system response (sometimes called the “Rest and Digest Response”) meant to counter the negative effects of autonomic arousal. CBT aims to train our bodies to switch over to this relaxing state by engaging in activities such as diaphragmatic breathing, progressive muscle relaxation, and guided imagery.
Research has shown CBT to be effective in improving bowel symptoms, psychological distress, and quality of life. Research studies have found that CBT can be helpful for about 1 in 3 people – there is ongoing research in this area and further studies are needed to determine the best approaches for different patients.
Follow us at http://www.facebook/com/getcandorapp