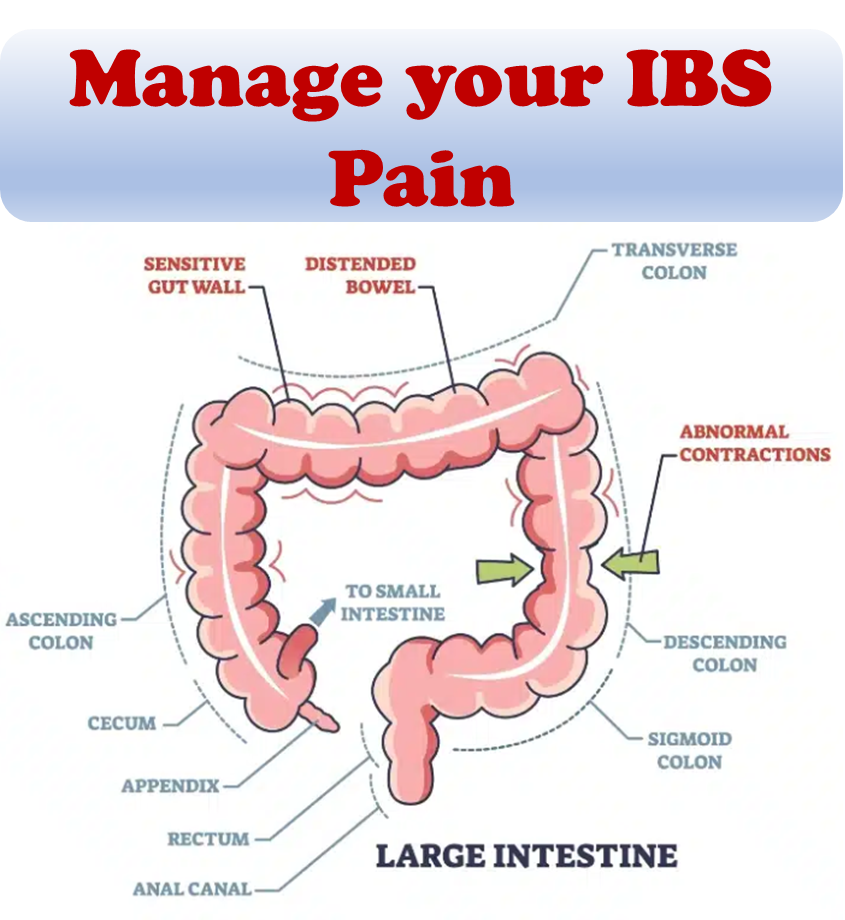
Living with Irritable Bowel Syndrome (IBS) poses daily challenges, especially in navigating dietary choices. While it is important to know the common IBS trigger foods, understanding the nuances of individual responses to these foods is crucial.

Common Trigger Foods:
- Greasy Food:
The impact of high-fat content on the gastrocolic reflex can exacerbate IBS symptoms. Foods like pizza, fried items, and fatty meats may be problematic for those with sensitive digestive systems. Opting for lean sources of healthy fats, such as fish, nuts, and avocados, can contribute positively to digestive health. Moreover, exploring cooking methods that minimize added fats can be beneficial. - Dairy Products:
Lactose intolerance, affecting the digestion of dairy sugars, can lead to bloating and cramping. Options like lactose-free milk and low-lactose cheeses may be more tolerable. Incorporating fermented dairy products like yogurt with active cultures not only provides essential nutrients but also contributes to a healthier gut microbiome. - High-FODMAP Fruits:
Certain fruits high in fermentable carbohydrates (FODMAPs) can pose challenges. While apples and cherries might be problematic, low-FODMAP alternatives like bananas and blueberries may be better tolerated. Recognizing that cooking fruits may make them easier for the system to handle can provide additional dietary flexibility. Experimenting with various preparation methods can help identify what works best. - High-FODMAP Vegetables:
Similar to fruits, some vegetables rich in FODMAPs may contribute to IBS symptoms. Balancing the intake of these vegetables with cooked or juiced options can be beneficial. It’s essential to note that while limiting certain vegetables, others, such as carrots and zucchini, are generally well-tolerated. Exploring diverse cooking techniques, such as steaming or roasting, can enhance digestibility. - Wheat:
Gluten-containing grains, even without celiac disease, may cause issues due to the presence of fructans. Gluten-free alternatives are readily available and can be explored. Incorporating whole grains like quinoa and rice can still provide necessary dietary fiber without triggering symptoms. Additionally, exploring a variety of gluten-free grains, such as millet or buckwheat, can add diversity to the diet.
It is crucial to look beyond a simple listing of trigger foods to promote a deeper understanding of their effects. Beyond identifying potential culprits, look for practical alternatives and cooking methods, emphasizing the importance of personalized approaches.
- Beans and Legumes:
Beans and legumes, rich in poorly digested carbohydrates, can lead to intestinal gas. Exploring well-rinsed, canned options may be an alternative for vegetarians. Additionally, incorporating other protein sources like tofu or lean meats can help meet nutritional needs without exacerbating symptoms. Experimenting with different cooking methods, such as soaking and slow cooking, can enhance digestibility. - Spicy Foods:
Studies suggest that spicy foods, particularly those containing chili peppers, may contribute to abdominal pain in individuals with IBS. Experimenting with milder spices or herbs as alternatives can add flavor without the potential for symptom aggravation. Understanding individual spice tolerances and gradually introducing them into the diet can help identify personal thresholds. - Sugar Substitutes:
Artificial sweeteners and sugar alcohols, found in various sugar-free products, may be poorly tolerated. Opting for sweeteners like stevia or maple syrup could be alternatives. Understanding the impact of sugar substitutes on the gut microbiome is an evolving area of research, and moderation is key. Additionally, exploring natural sweeteners like honey or agave syrup can offer alternatives with potentially fewer digestive implications. - Soda:
Carbonated drinks can contribute to gas and bloating, with the high sugar content potentially impacting gut bacteria. Healthier alternatives include water, iced tea, or diluted cranberry juice. Staying hydrated with water is particularly crucial for overall digestive health. Experimenting with herbal teas or infused water can add variety to beverage choices. - Alcohol:
Some alcoholic beverages, particularly rum, are high in FODMAPs. Moderate consumption, such as small amounts of red wine, may be a safer choice. Choosing clear spirits and diluting with water or mixers low in FODMAPs can be alternatives for those who enjoy an occasional drink. Experimenting with different types of alcoholic beverages and monitoring individual responses can help tailor alcohol choices to personal tolerance levels. - Caffeine:
Caffeine, known as an IBS trigger for some, can lead to symptoms like dyspepsia and loose stools. Gradual reduction in caffeine intake may be worth exploring. Experimenting with alternative caffeine sources like green tea, which contains lower caffeine levels, can be a suitable adjustment. Additionally, considering factors such as the timing of caffeine consumption and the impact on daily routines can contribute to effective management.
Understanding and managing IBS involves a nuanced approach to identifying personal triggers. Keeping a detailed food diary can aid in pinpointing specific foods that affect individual symptoms. Additionally, recognizing the role of FODMAPs, moderating alcohol and caffeine intake, and choosing alternatives can contribute to better IBS management.
References:
- Varney J, Barrett J, Scarlata K, Catsos P, Gibson PR, Muir JG. (2017) “FODMAPs: food composition, defining cutoff values and international application.” Journal of Gastroenterology and Hepatology.
- Volta U, Pinto-Sanchez MI, Boschetti E, Caio G, De Giorgio R, Verdu EF. (2016) “Dietary triggers in irritable bowel syndrome: Is there a role for gluten?” Journal of Neurogastroenterology and Motility.
- Cozma-Petruţ A, Loghin F, Miere D, Dumitraşcu DL. (2017) “Diet in irritable bowel syndrome: What to recommend, not what to forbid to patients!” World Journal of Gastroenterology.
- Johns Hopkins Medicine. Facts about sugar and sugar substitutes.
- Ruiz-Ojeda FJ, Plaza-Díaz J, Sáez-Lara MJ, Gil A. (2019) “Effects of sweeteners on the gut microbiota: A review of experimental studies and clinical trials.” Advances in Nutrition.
- Reding KW, Cain KC, Jarrett ME, Eugenio MD, Heitkemper MM. (2013) “Relationship between patterns of alcohol consumption and gastrointestinal symptoms among patients with irritable bowel syndrome.” American Journal of Gastroenterology.